Ask any HIV researcher, employee of an HIV/AIDS organization or HIV activist what the most significant development in eliminating the virus in the last several years has been, and odds are they will say Pre-Exposure Prophylaxis, or PrEP.
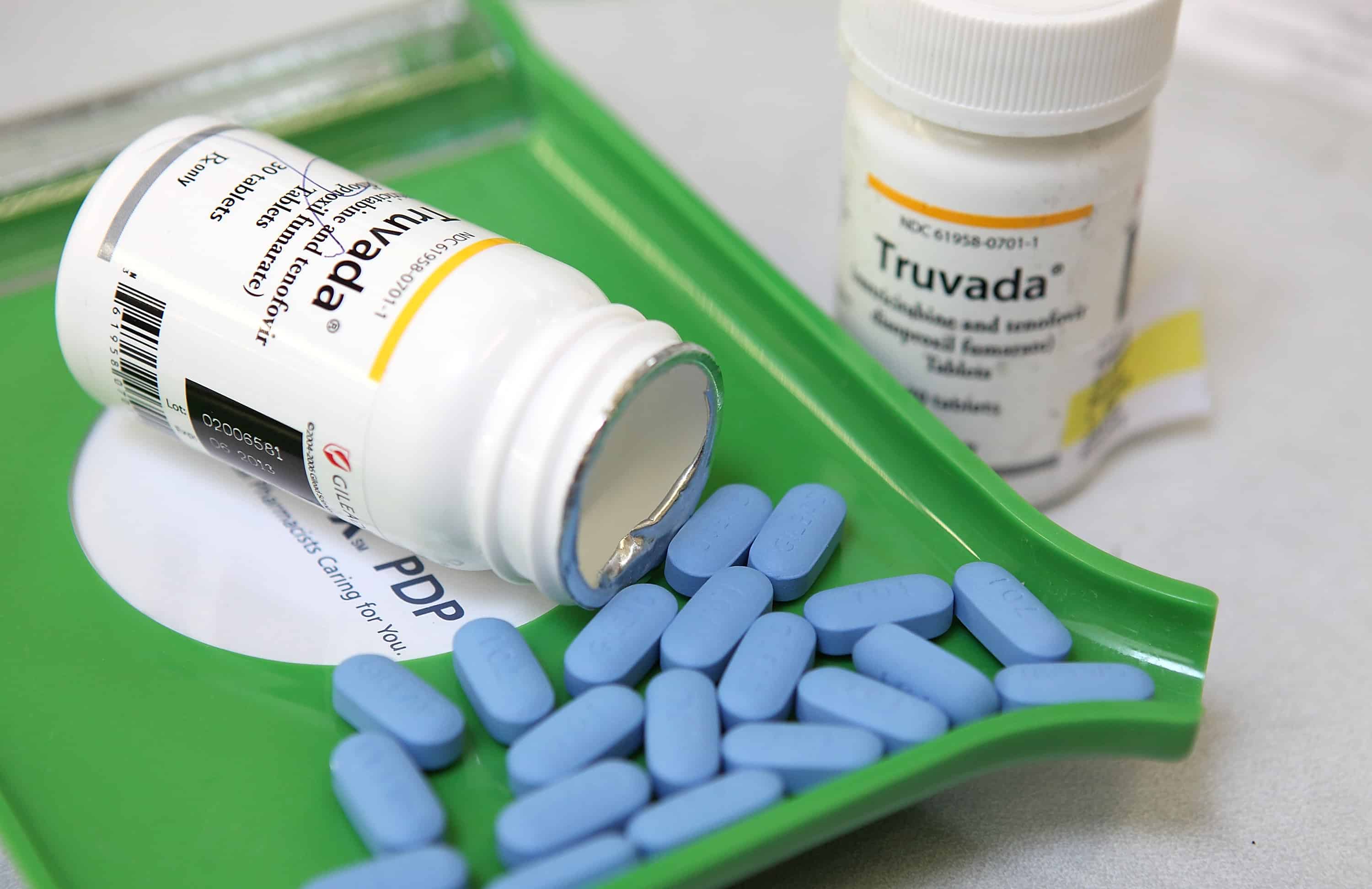
PrEP is s a way for people who do not have HIV but who are at substantial risk of getting it to prevent HIV infection by taking a pill every day. That pill’s brand name is Truvada, and studies have shown that if taken every day the pill is more than 90 percent effective in preventing contracting HIV.
Despite the growing conversation and near-unanimous medical and scientific approval of the regimen, there remains a disconnect over how to get it, and more importantly, how not to spend a fortune doing so.
More and more Atlanta-area organizations and medical practices are offering, or plan to offer, PrEP, and they are doing so while clearing a path that will allow individuals to get it nearly, and in many cases completely, free of charge.
CDC recommendation sent PrEP demand into overdrive
The Food and Drug Administration approved Truvada in the summer of 2012, and it is currently the only drug recommended for the PrEP regimen. But the attention paid to it picked up last May, when the U.S. Public Health Service released new federal PrEP guidelines, developed by a working group led by the Centers for Disease Control and Prevention, recommending PrEP for people who are at a substantial risk for HIV infection, including gay and bisexual men and transgender women.
That move put the push for offering the option of PrEP into overdrive. Most organizations, including the Fulton County Department of Health and Wellness and the AIDS Research Consortium of Atlanta, recommend that individuals interested in taking PrEP first ask their primary care physicians about it. But some people have experienced difficulties receiving the drug, for a variety of reasons. This fact troubles AIDS Research Consortium of Atlanta principal investigator Dr. Melanie Thompson.
“If you are uncomfortable talking about sexual health and HIV risk with your doctor, then my next question would be ‘Is this the right doctor for you?’” Thompson says. “To receive appropriate and comprehensive health care, you must be able to discuss intimate issues with your provider.”
She says people often find that their doctors are open to having such conversations, but may be less comfortable initiating them. If you’ve tried and felt let down, consider looking elsewhere she says.
“Sadly, many doctors often are not ‘culturally competent’ in dealing with issues about sexuality and HIV/STI prevention, especially for LGBT persons,” Thompson says.
She recommends using The Health Initiative’s provider directory of LGBT-friendly physicians to find more progressive options.
‘Cost should not be a barrier to people getting PrEP’
To fill in the gaps and spread the word, HIV/AIDS organizations around town are busy working to educate and provide options for PrEP.
AID Atlanta will begin offering PrEP in February or March at the latest, according to Craig Washington, AID Atlanta’s prevention programs manager. Michael Baker, Positive Impact’s director of advancement, says that while his organization is not currently funded to offer PrEP, it is actively creating referral networks and other funding sources to potentially offer it to clients in the future.
LGBT-friendly medical practices like AbsoluteCARE and Pride Medical are offering PrEP right now, and all the organizations, medical practices and health departments the GA Voice spoke to detailed ways to get the drug for next to nothing.
The suggested monthly wholesale price for Truvada is roughly $1,500. However, prices in the Atlanta area have ranged from $1,300 to $1,500 per month, according to ARCA’s Thompson. That’s the price most individuals interested in the regimen have assumed they will have to pay. But that’s not entirely the case.
Truvada is listed as a Tier 4, 5 or specialty drug on most insurance plans, which means instead of a flat copay, a person would pay a percentage of the cost (called co-insurance), which can range from 10 to 50 percent, according to Thompson. So for a $1,400 prescription with 20 percent co-insurance, the patient would be responsible for $280 per month.
Those who have private insurance can get a $300 per month copay card for Truvada from their care provider or from the Truvada website, Thompson says. So in the example given above, a person would end up paying nothing. However, copay cards cannot be used with Medicare drug programs, and you must have an HIV test every three months to continue on the copay assistance plan for PrEP.
Dr. David Morris, medical director at Pride Medical, says that the average patient of theirs with insurance is able to get PrEP for between zero and $30 per month.
“We get insurance companies to pay for it and Gilead [the company that manufactures Truvada] to pick up the cost of the copay,” he says. “Cost should not be a barrier to people getting PrEP.”
But what about those who are uninsured? Gilead has a patient assistance program that provides the drug free of charge if:
• You’re a U.S. resident and have proof of residency
• Have a physician that will prescribe the medication
• Have an annual income under 500 percent of the poverty level (a one-person household with an income under $58,350, according to Mercedes Wilkinson at the Fulton County Department of Health and Wellness)
Those who meet the criteria qualify for six months of medication for free, with eligibility for renewal after six months. Gilead will also contact a physician’s office every month when a person is due for a refill to make sure the prescription is needed and to verify a negative HIV test is on file for the previous 90 days. The medication will be shipped directly to the physician, so medication appointment fees may apply, depending on the physician’s rates.
‘It’s not about pushing PrEP for PrEP’s sake’
While the path to cost-free PrEP appears closer and closer to a reality for many, the experts caution the drug isn’t for everyone, even for those who are HIV-negative, sexually active and are a gay or bisexual man or in any other group at a higher risk for contracting the virus.
Most physicians and health organizations will run a series of tests in addition to an HIV test, including blood work and kidney function.
“It’s a drug like any other, so we want to make sure people are well-suited to take the regimen,” says AID Atlanta’s Washington. HIV tests will be administered every three months.
Many health care experts and HIV activists agree that education on PrEP should not be limited to the general public looking to begin the regimen.
“I think we need a statewide training initiative where we’re doing due diligence and training the providers, particularly the primary care physicians,” Washington says. “It’s not about pushing PrEP for PrEP’s sake. There is the task at hand of giving people an even more informed choice.”
Thompson agrees, saying, “Bottom line: PrEP is a valuable tool that we are just learning to use.”
PrEP Resources
PrePWatch: www.prepwatch.org
My PrEP Experience: myprepexperience.blogspot.com
PrEP Facts: prepfacts.org
GoodRx: www.goodrx.com/truvada
Gilead Sciences PrEP Page: start.truvada.com
Gilead Science Medication Assistance: 855-330-5479
Truvada co-pay assistance: www.truvada.com/truvada-patient-assistance